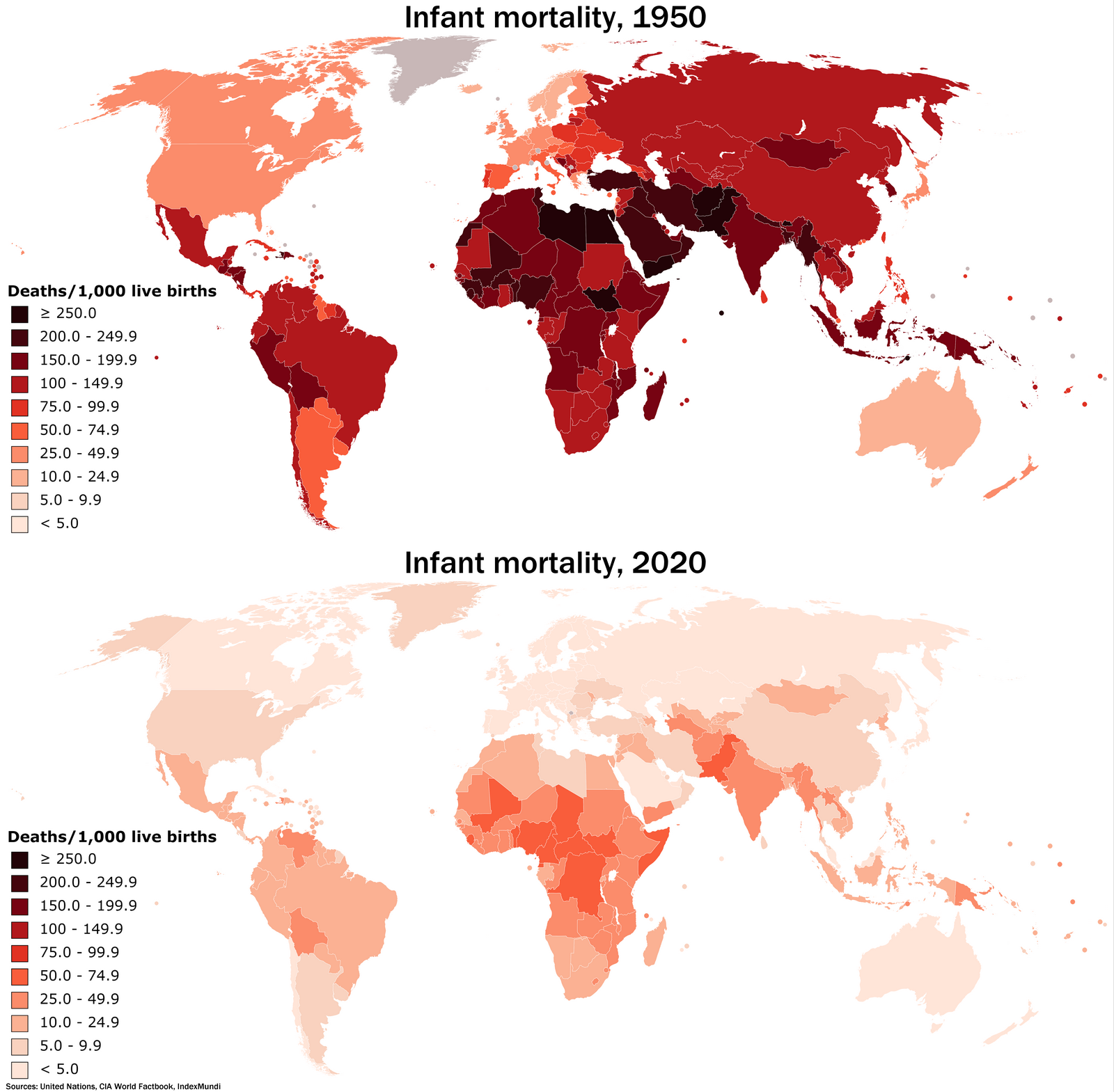
Infant mortality rates remain a critical issue in public health, reflecting broader disparities in healthcare access and quality. Recent studies reveal alarming trends, showing that Black infants continue to die at rates significantly higher than their white counterparts. While overall life expectancy has improved across racial lines, the stark contrast in infant death rates highlights systemic inequalities that persist in the United States. Factors contributing to these disparities include healthcare inequality and socioeconomic influences, which compound the challenges facing marginalized communities. Addressing the racial health gaps that contribute to these tragic outcomes is paramount for achieving equity in healthcare and ensuring a healthier future for all infants.
The rates at which infants do not survive through their first year is a pressing concern that underscores ongoing healthcare challenges within society. When examining the broader scope of mortality outcomes, one finds that certain groups, particularly Black infants, face significantly higher death rates compared to white infants. Despite advancements in medical care and increased life expectancy, certain severe disparities remain persistent and troubling. The challenges associated with prenatal care, infant health interventions, and health service accessibility reveal a multifaceted problem tied to economic, social, and racial health dynamics. Consequentially, addressing these critical disparities not only serves to improve individual lives but also strengthens the fabric of public health overall.
The Alarming Disparity in Infant Mortality Rates
The findings from the recent study are stark: Black infants are dying at rates significantly higher than their white counterparts, with current figures showing that Black infant mortality rates are now twice that of white infants. This alarming statistic underscores a persistent healthcare inequality that has not just remained stagnant but has indeed worsened over the last seven decades. Despite notable improvements in life expectancy for both Black and white Americans, this troubling disparity emphasizes the critical need for targeted public health strategies to address these underlying issues. The rise of infant mortality rates among Black infants is a cry for urgent action.
Research has shown that the leading causes of infant death often stem from medical conditions related to pregnancy and childbirth. Such complications are exacerbated by systemic barriers that disproportionately affect Black families, revealing deep-seated disparities in access to quality healthcare. These inequalities are multilayered, involving socio-economic factors, types of care received, and community resources. Addressing these disparities is not merely about improving statistics but about ensuring equitable access to healthcare for all families, regardless of race.
Understanding Healthcare Inequality in America
The widening gap in infant mortality rates signals a broad spectrum of healthcare inequality that cannot be ignored. While policymakers and healthcare advocates tout the improvements seen in life expectancy and general healthcare metrics, the data reveals a sobering truth — not all populations are benefiting equally. Black Americans, particularly infants, continue to bear the brunt of these disparities. This healthcare inequality demands a critical examination of systemic factors that contribute to poorer outcomes for Black infants, including socio-economic status, geography, and the healthcare system’s responsiveness to the needs of these communities.
Healthcare inequality is further complicated by factors such as implicit biases within the medical system and a lack of culturally competent care. The differences in the quality of care that patients receive can lead to significant health outcomes disparities. For instance, Black mothers may not receive the same level of pre-natal care due to historical mistrust of the healthcare system and social determinants of health. To bridge this gap, it is essential to foster a healthcare environment that prioritizes equity and is responsive to the diverse needs of all patients.
Longitudinal Insights into Racial Health Gaps
This study’s longitudinal approach, analyzing data over a span of 70 years, allows for a comprehensive understanding of changes in healthcare outcomes and, importantly, the persistent racial health gaps in America. Although overall mortality rates for both Black and white Americans have improved, the disparities in infant mortality have remained stark and indeed worsened for Black infants. Longitudinal studies provide critical insights that shorter analyses might overlook, exposing the continued systemic issues that endanger the lives of Black infants now at an alarming rate compared to their white peers.
Moreover, this expansive timeframe reveals trends and patterns that highlight the necessity for ongoing vigilance and intervention strategies. By reflecting on historical data, stakeholders can better identify the factors contributing to Black infant mortality, thus allowing for more effective policy responses. It’s imperative that healthcare policy reforms address both historical injustices as well as current inequalities to create a health climate where every infant has the opportunity to thrive, regardless of racial or socio-economic background.
Comparative Life Expectancy: A Minor Victory or Major Oversight?
While it’s undeniable that life expectancy has generally increased for both Black and white Americans, this statistic can mask the persistent and even growing disparities that exist, especially among infants. The fact that Black adults have witnessed an 18 percent higher mortality rate underscores that progress does not translate to uniform improvement across racial lines. Life expectancy statistics should provoke critical discussions about what they truly reflect. Are we satisfied simply because some groups are faring better while others continue to struggle? This question begs further investigation into the equity of health resources and outcomes.
When discussing life expectancy, we must examine the underlying factors that contribute to these rates. Differences in healthcare access, quality of care, and social determinants of health play pivotal roles in shaping outcomes. While Black adults are living longer than in previous decades, the stark contrast in life expectancies for Black infants highlights the need for more targeted solutions. Public health initiatives must pivot from generalized improvements to addressing the specific needs and challenges faced by Black communities to make equal strides across all demographics.
Addressing Disparities Through Policy Change
In light of the alarming findings regarding Black infant mortality rates, there is a clarion call for policy changes that prioritize health equity. Policymakers must focus on crafting solutions that specifically address the factors contributing to higher mortality rates in Black infants. This involves not only increasing healthcare access but also ensuring that quality of care is consistent and culturally competent. Public health campaigns should aim to increase awareness of maternal and infant health issues within Black communities, engaging with families to understand their needs better.
It is essential for legislators and health officials to recognize that the current trajectory allows systemic inequalities to persist, negatively impacting Black infants and families. Strategies to improve prenatal and postnatal care must be implemented with urgency, including funding for healthcare programs that serve vulnerable populations. By pushing for reforms that address these disparities, we can begin to level the playing field and significantly improve outcomes for Black infants, ultimately working toward the goal of equity in health for all.
The Role of Community Engagement in Health Solutions
Community engagement is a crucial component in addressing disparities in infant mortality rates. Empowering local communities to participate in health initiatives fosters ownership and encourages changes that are culturally relevant. By involving community members in designing and implementing health programs, we can better tailor solutions to meet the unique needs of Black families, thus helping to diminish racial health gaps. These grassroots efforts can also improve trust levels within the healthcare system, ensuring that families feel valued and heard.
Additionally, community health workers can play a pivotal role in bridging the gap between healthcare providers and patients. They are often the voices of the community and can facilitate access to necessary resources. Their involvement ensures that prenatal and infant care initiatives are not only accessible but also resonate with those they serve. Investing in community health resources is a promising step toward reducing healthcare inequalities and improving the overall health of Black infants, ultimately leading to a decline in the concerning mortality rates seen today.
The Ongoing Impact of Socio-Economic Factors on Infant Health
Socio-economic factors are critical to understanding the disparities in infant mortality rates. Issues such as poverty, education, and access to nutritious food create environments where Black infants are more at risk. The intersection of these factors often leads to inadequate healthcare access, which can severely impact pregnancy outcomes. This socio-economic landscape must be addressed through comprehensive policies that aim to uplift the entire community, ensuring that all families have the resources they need to thrive.
Moreover, addressing socio-economic disparities isn’t just a matter of health; it’s a matter of justice. Ensuring that Black families have equitable access to healthcare and supportive resources can fundamentally alter their health trajectories. Policies that prioritize economic equality—whether through job opportunities, educational initiatives, or healthcare access—will ultimately contribute to improved health outcomes for Black infants, thereby working towards closing the widening gap in infant mortality rates.
Future Research Directions: Unpacking Causes of Disparities
To effectively combat the ongoing disparities in infant mortality rates, future research must prioritize identifying and unpacking the underlying causes. While current findings highlight the stark differences in outcomes between Black and white infants, understanding the nuanced factors contributing to these disparities is essential. This includes examining healthcare access, potential biases in treatment, and the broader socio-political environment that loads the dice against Black mothers and their infants.
Moreover, studies should focus on the lived experiences of families affected by these inequities. By incorporating qualitative research that captures the voices of those most impacted, we can gain insights that may be overlooked in quantitative analyses. This approach will not only enrich our understanding of the disparities but also guide effective interventions that resonate with the communities in need, ultimately striving towards a future where every infant has the chance to thrive, regardless of their racial background.
Frequently Asked Questions
What are the current disparities in infant mortality rates between Black and white infants?
Recent studies indicate that Black infants die at twice the rate of white infants, with a disparity that has widened from a 92% higher mortality rate in the 1950s to a staggering 115% today. This highlights significant healthcare inequalities that require urgent attention.
How have healthcare inequalities contributed to rising infant mortality rates for Black infants?
Healthcare inequalities, characterized by unequal access to quality medical care, are pivotal in the rising infant mortality rates among Black infants. Factors such as inadequate prenatal care, underlying health conditions, and socio-economic status contribute to these disparities.
Why has the gap in infant mortality rates not improved despite advancements in healthcare?
Although overall life expectancy has improved for both Black and white Americans, the infant mortality rate disparity has worsened. This paradox suggests that healthcare advancements are not equitably benefiting all racial groups, particularly Black infants who continue to face systemic obstacles.
What factors were identified as leading causes of excess infant deaths in Black infants?
The study identified medical conditions during pregnancy as the leading cause of excess death among Black infants. This indicates a need for targeted prenatal care and interventions to address specific health challenges faced by expectant Black mothers.
What does the research say about life expectancy comparisons between Black and white Americans?
While life expectancy for both Black and white Americans has improved since the 1950s—with Black Americans improving from 60.5 years to 76 years—the racial health gaps remain pronounced, especially in infant mortality rates, highlighting ongoing health disparities.
How many lives could potentially have been saved if Black Americans had equal healthcare resources as white Americans?
The research suggests that around 5 million Black American lives could have been saved over the past 70 years if they had access to the same healthcare resources as their white counterparts, underscoring the critical need for policy changes.
What actions should policymakers take to address disparities in infant mortality rates?
Policymakers need to prioritize access to quality healthcare, enhance prenatal services, and focus on the systemic issues contributing to healthcare inequality. Targeted interventions aimed at reducing disparities in infant mortality rates are crucial for achieving health equity.
What role does the time span of studies play in understanding disparities in infant mortality rates?
Longitudinal studies covering multiple decades offer a more comprehensive view of how disparities in infant mortality rates have evolved. Shorter studies may fail to capture the persistent problems that affect specific racial groups, thereby obscuring critical insights.
What are the long-term trends in healthcare outcomes for Black infants compared to white infants?
Long-term trends indicate that while healthcare outcomes for Black infants have seen some improvements, the relative gaps in infant mortality rates compared to white infants have significantly widened, pointing to deep-rooted systemic disparities.
| Key Points |
|---|
| Mortality rates have improved for Black and white Americans overall, but not for infants. |
| Black infants die at twice the rate of white infants. |
| Life expectancy for Black Americans has increased from 60.5 years in the 1950s to 76 years in the 2010s. |
| Life expectancy for white Americans has increased from 69 years in the 1950s to 79.3 years in the 2010s. |
| The racial gap in mortality has narrowed, but Black adults still have an 18% higher mortality rate compared to white adults. |
| The disparity in infant mortality increased from 92% higher for Black infants in the 1950s to 115% today. |
| Medical conditions during pregnancy are the leading cause of excess deaths among Black infants in the 2010s. |
Summary
Infant mortality rates are a critical indicator of a nation’s health, and current findings reveal alarming disparities between Black and white infants. Despite overall improvements in life expectancy since the 1950s, the infant mortality gap has widened, with Black infants facing a mortality rate that is twice as high as that of their white counterparts. This concerning trend emphasizes the need for targeted public health policies to address the underlying causes of these disparities and ensure equitable healthcare access for all infants.